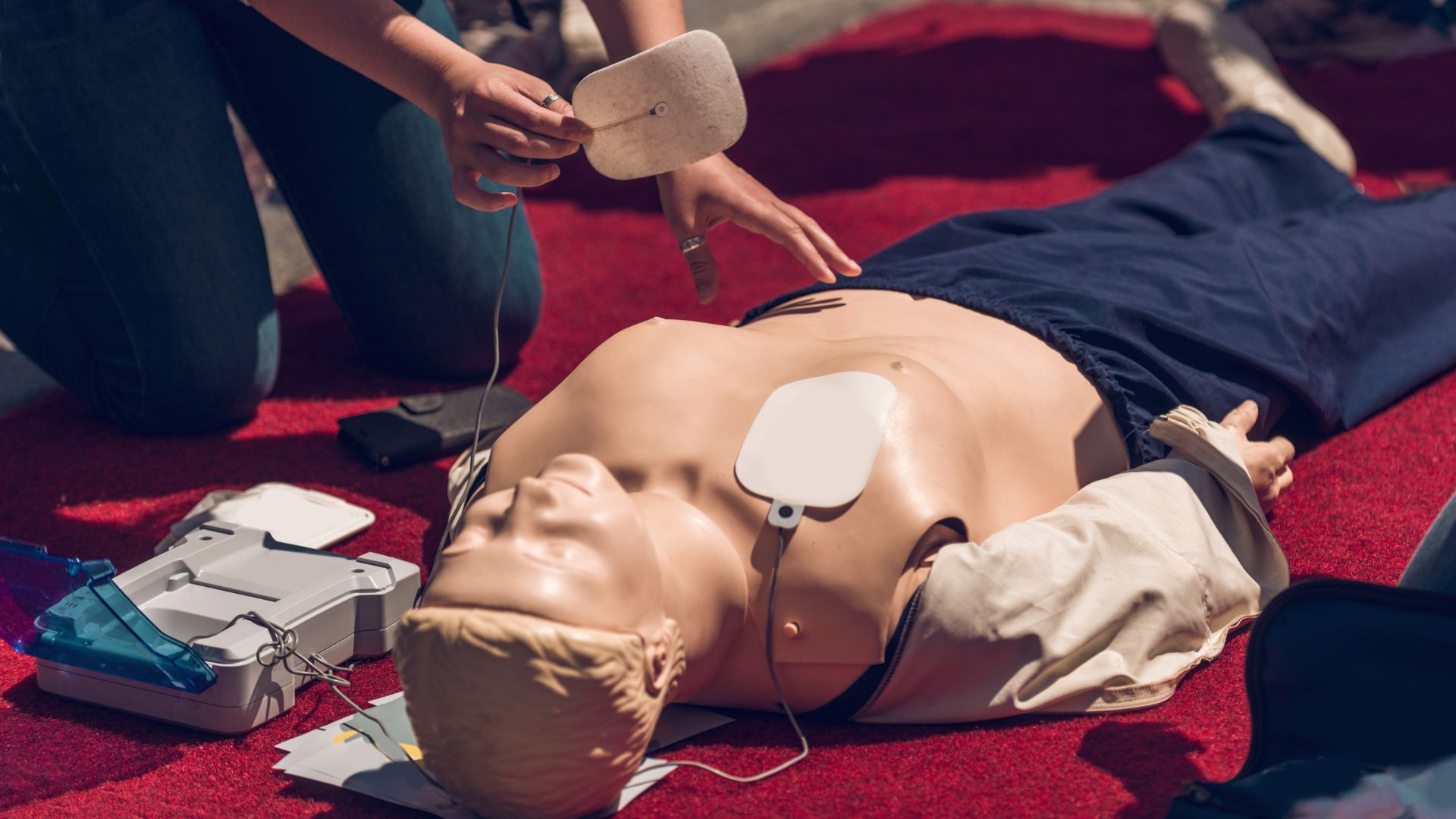
In times of medical emergencies, defibrillators play a crucial role in saving lives. They’re designed to restore the heart’s normal rhythm when someone experiences cardiac arrest. But what is a defibrillator, and how does it work exactly?
There are so many myths that stop individuals from learning how to use defibrillators, such as the one where they think they’re too complicated. However, this couldn’t be more far from the truth. To help you understand why these devices are so effective, let’s explore the ins and outs of defibrillators, the different types that exist, and the step-by-step process of using them.
Cardiac Arrest 101
Before understanding the way defibrillators work, let’s first understand what happens during cardiac arrest. Cardiac arrest occurs when the heart’s electrical system malfunctions. This causes the heart to stop beating effectively. What happens is an interruption of blood flow to the vital organs, such as the brain, which can quickly lead to irreversible damage or death.
Many factors can cause cardiac arrest, including heart disease, trauma, drug overdose, drowning, or electric shock. It’s important to note that cardiac arrest is different from a heart attack, which is a blockage of blood flow to a part of the heart muscle.
When someone experiences cardiac arrest, they lose consciousness and stop breathing or gasp for air. The only effective treatment in this case is to restore the normal rhythm of the heart with an electric shock called defibrillation.
What Is a Defibrillator and How Does It Work?
Defibrillators are designed to treat life-threatening arrhythmias, particularly ventricular fibrillation and ventricular tachycardia. Both these conditions disrupt the heart’s normal electrical activity. They cause it to beat irregularly and prevent it from effectively pumping blood.
A defibrillator delivers an electric shock to the heart of a person who is experiencing a cardiac event. First, defibrillators detect the heart rhythm of the person. Then, they use that information to deliver a precise electrical shock if needed. The shock can restore a normal heart rhythm and allow the heart to resume pumping blood.
Different types of defibrillators exist, ranging from “smart” ones, which can be used outside of hospitals, through hospital-grade super powerful ones, to implanted defibrillators. Regardless of type, the point of a defibrillator is to get the heart to contract rhythmically again by jump-starting its flailing electrical system.
Different Types of Defibrillators
Let’s get into the details. There are several different types of defibrillators, such as manual, automated, implantable, and wearable. Each type has its own pros and cons, depending on the situation and the person’s medical history. Let’s take a look at the most common types:
External Defibrillators
You’ll find that external defibrillators are used in various settings, including hospitals, public spaces, and even homes. They come in two main forms: automated external defibrillators (AEDs) and manual defibrillators.
Automated External Defibrillators (AEDs)
AEDs are user-friendly devices. Anyone can operate with them, regardless of their medical training. AEDs are equipped with adhesive pads or paddles that are placed on the patient’s chest, which is how they analyze the heart’s rhythm and deliver an electric shock if necessary.
One of the key advantages of AEDs is their ability to provide clear verbal instructions to guide you through the entire process. This feature is particularly useful in high-stress situations where quick action is crucial. AEDs have already proven to be lifesavers in public spaces, such as airports and shopping malls, where immediate access to medical assistance is essential.
Manual Defibrillators
Healthcare professionals with specialized training typically use manual defibrillators. They allow the medical personnel to have more control over the energy level and timing of the shocks delivered to the patient. Manual defibrillators are commonly found in hospitals, ambulances, and other healthcare settings.
Implantable Cardioverter Defibrillators (ICDs)
Implantable cardioverter defibrillators (ICDs) are surgically implanted devices used for patients at high risk of recurrent arrhythmias or sudden cardiac arrest. They continuously monitor the heart’s rhythm and provide immediate intervention if an abnormal rhythm is detected. ICDs are highly beneficial for individuals with underlying heart conditions or a history of cardiac events.
Wearable Cardioverter Defibrillators (WCDs)
Wearable cardioverter defibrillators (WCDs) are portable devices worn by patients who are at high risk of sudden cardiac arrest but aren’t suitable candidates for implantable devices. WCDs continuously monitor the heart’s rhythm and can deliver a shock if necessary. They provide temporary protection until a more permanent solution, such as an ICD, can be implemented.
The Defibrillation Process
Cardiac defibrillation refers to a process that stops the fibrillation of the wall of the heart’s chambers. When the heart’s muscles flicker instead of contracting, the heart cannot pump blood. This is known as fibrillation and is exactly the condition that defibrillators address.
Whether it is a manual or an AED, here’s how you can use it:
1. Preparation
Before using a defibrillator, it’s crucial to ensure the safety of both the patient and the rescuer – confirming the absence of any conductive materials, such as water or metal, that could interfere with the delivery of the electric shock. It’s also important to ensure that no one is touching the victim or the surrounding surface, especially if it’s conductive, during the defibrillation process.
2. Placement of Pads or Paddles
Next, you place the defibrillator pads or paddles on the patient’s chest. The exact placement may vary depending on the specific device being used, as AEDs use pads, while manual defibrillators have paddles. One pad or paddle goes below the right shoulder, and the other one below the left nipple. These pads or paddles contain conducting material to prevent burns and facilitate the transmission of the electric shock.
3. Analysis of Heart Rhythm
Once you properly position the pads or paddles, the defibrillator will analyze the patient’s heart rhythm. This analysis can determine whether a shock is required to restore normal rhythm. AEDs are equipped with advanced algorithms that can quickly and accurately assess the heart’s electrical activity. It determines when and whether a shock is required.
4. Delivery of Electric Shock
If the defibrillator detects a shockable rhythm, it will prompt you to deliver the electric shock. In the case of an AED, a button is pressed to initiate the shock, while manual defibrillators require you to press the buttons on the handles of both paddles simultaneously.
The electric shock itself is delivered in a controlled manner, causing the heart muscle to stop its activity, thus allowing it to reset momentarily. As the operator, you’re the one who determines the amplitude of the shock.
5. Monitoring and Follow-up
After delivering the electric shock, the healthcare provider or rescuer will continue with cardiopulmonary resuscitation (CPR) for a specified period, usually two minutes. This helps maintain blood circulation and oxygenation while allowing the heart to recover and potentially resume normal rhythm. The provider will then reassess the patient’s pulse and heart rhythm to determine if additional shocks or interventions are necessary.
Common Misconceptions About Defibrillation
Since we answered what a defibrillator is and how it works, let’s now address a few common myths that are often seen in association with using them:
Defibrillators Restart a Stopped Heart
Contrary to popular belief, defibrillators don’t restart a heart that has completely stopped. Instead, you use them with the hopes of restoring the heart’s normal rhythm when it’s in a state of abnormal electrical activity, such as ventricular fibrillation or ventricular tachycardia.
In cases where the heart has ceased all electrical activity, defibrillation alone isn’t effective, and additional medical interventions are required, like CPR.
Defibrillators Cause Harm
While defibrillators deliver a powerful electric shock, they’re designed to be safe and effective when used correctly. Modern defibrillators, especially AEDs, are equipped with advanced technologies that ensure the delivery of appropriate energy levels. They’ll also provide clear instructions to guide you through the process, which minimizes the risk of user error.
CPR Replaces the Need for Defibrillation
Cardiopulmonary resuscitation (CPR) is a vital life-saving technique that helps maintain blood circulation and oxygenation until a defibrillator is available. However, CPR alone cannot restore a normal heart rhythm. Defibrillation is necessary to reset the heart’s electrical activity and increase the chances of successful resuscitation. They work best when used together.
Conclusion
So, what Is a defibrillator, and how does it work? Answering this question isn’t a task we take lightly. We want to show you exactly why defibrillators are invaluable tools when treating cardiac arrest victims. So, by dispelling common misconceptions and explaining how defibrillators work, we hope to empower each one of you to take action.
If you’re looking to put your newfound defibrillation knowledge to good use, it’s time to get yourself a CPR certification in Lanham and learn one more vital skill you’ll be proud of.